According to a new study, 228 clinical procedures are being utilized incorrectly in Canada, with underuse being more common than excess.
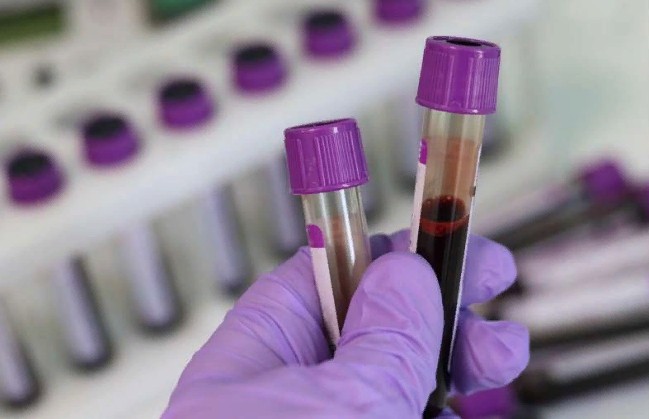
Diagnostic and therapeutic procedures such as blood testing and radiographs are included in this list. The study, which was published in the Canadian Medical Association Journal, can help health care providers, organizations, and governments enhance patient care and results.
Dr. Janet Squires, a professor of nursing at the University of Ottawa and a senior scientist at The Ottawa Hospital, and coauthors write, “The main result from our research is that there are huge gaps between the treatment patients should receive and the care they do receive.”
“We discovered that, on average, 30.0 percent of care obtained by Canadians was deemed inappropriate, as assessed in the included research publications using the Institute of Medicine’s categories of underuse and overuse.”
The researchers looked at 174 articles to see if clinical practices in Canada followed evidence-based guidelines. Between 2007 and 2021, these trials comprised 228 clinical practices and analyzed over 28.9 million participants.
In diagnostics and therapeutics, the researchers discovered inappropriate care in 30% of instances, with a median score of 44% for underuse and 14% for overuse in diagnostics and therapeutics.
Glycated hemoglobin testing, lipid panel blood tests, and diabetic eye exams were all underutilized diagnoses. Thyroid-stimulating hormone blood tests, chest radiography, and Pap tests were the most commonly misused diagnostics.
Inappropriate treatment can result in injury from the use or lack of use of a therapy or diagnostic technique, as well as unfavorable patient experiences, poor health outcomes, and inefficient use of scarce healthcare resources.
“We discovered that many clinical procedures obtained by patients in Canada are inappropriate,” the authors write. “Whether the practice is diagnostic or therapeutic, it commonly fails to satisfy suggested standards.”
They advise that these findings be used by provincial and territorial governments, as well as quality improvement organizations, to improve health care quality and perform future studies. Clinicians can use the list of clinical practices, particularly the top 42 most-studied practices, to choose which practices should be changed first.
Dr. Kaveh Shojania, a general internist at Sunnybrook Health Sciences Centre, suggests that refocusing priorities on social determinants of health such as housing, education, air and water quality, early childhood development, and more could have a greater impact than narrower system changes in a related commentary.
Given the huge challenges the health system is facing from the COVID-19 pandemic, the opioid epidemic, and other threats, this perspective is extremely critical.
Dr. Shojania states, “Interventions addressing these determinants would certainly yield higher returns on investment than generating tiny increases in the uptake of recommended practices that have largely small absolute health impacts.”